



|
Therapeutics and Possible Vaccine Used to Treat Covid-19: a Review
Muna O. Alamoudi1, Yousef F. Bakrshoom2, Saleh F. Bakrshoom3, Eitimad H. Abdel-Rahman1*, Hamdan S. Al-malky4, Isam M. Abu Zeid5 |
|
1 Biology Department, Faculty of Science, University of Hail PO Box 2240, Hai'l 81451, Saudi Arabia. 2Medical Department, Faculty of Medicine, University of Hail PO Box 2240, Hai'l 81451, Saudi Arabia. 3Physical Therapy Department, Faculty of Applied Medicine Science, University of Hail PO Box 2240, Hai'l 81451, Saudi Arabia. 4 Regional Drug Information Center, Ministry of Health, Jeddah 21442, Saudi Arabia 5 Department of Biological Sciences, Faculty of Sciences, King Abdulaziz University, PO Box 139109, Jeddah 21323, Saudi Arabia. |
ABSTRACT
Coronavirus disease 2019 (COVID-19) is an especially deadly respiratory disease caused by a severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection. It was first transmitted from animal to human in November 2019 in the open seafood market in Wuhan, and then from human to human, though the exact mode of transmission is not fully defined. This virus has spread throughout the world, and no effective vaccine or cure has been developed for it up to date. In this brief overview, we review a basic knowledge for COVID-19, its associated immune, pathology and histology, as well as available therapeutic approaches to provide clarification and future medically useful targets to grasp how COVID-19 co-circulates. The infection, prevention and supportive care for COVID-19 confirmed cases are the best-proven measures for the interventions until now; in addition, to use previous experience in the treatment of COVID-19 by various medicines for severe acute respiratory syndrome coronavirus (SARS-Cov), Middle East Respiratory Symptoms (MERS-CoV), Lupus, Anti-Malarial, Influenza Medicine, etc. were used to combat this disease. Nevertheless, various randomized trials of different drugs underway around the world can be used as a method for tracking the production of CVOID 19 vaccines, and interventions that continue worldwide. However, many vaccines are proposed by an international (privates and governmental bodies) trial against COVID-19. Therefore, the elimination of COVID-19 is an international priority, as the risk of disease will increase with increased death every day without viral spread control.
Key Words: COVID-19, Applied therapeutics, Proposed vaccine, Antiviral drugs.
INTRODUCTION
Viral infections are still of major complications worldwide [1-3]. At the end of 2019, a dangerous lung disease with unknown cause spread in Wuhan City, Hubei land, China [4] and on 12 January 2020 it was named Coronavirus 2019 (2019-nCoV). The disease was detected by the Chinese National Health Commission [5-7]. COVID-19 is one of the viruses that affects the lungs and can contribute to respiratory failure and death. A new SARS-CoV-2 (COVID-19) was detected in the human population after extreme Acute Respiratory Coronavirus Syndrome (SARS-CoV) and Middle East Respiratory Symptoms (MERS-CoV), resulting in a significant, widespread disease [8].
In March, [9] reported 87,137 patients from around the world, that represent 79,968 and 7,169 from inside and outside China, respectively who had a positive coronavirus test. The number of patients who died comes to 2873 and 105 deaths, which are 3.6% and 1.5% (rates at which people die) from inside and outside China, respectively [10]. The forced isolation in China has led to a fast decline in cases. Health and political authorities in northern Italy are then making extraordinary attempts in the peninsula to track the shock waves that are seriously affecting the health care system [11]. Many countries around the world have recorded more than 154 thousand deaths from 2.3 million cases of infection due to COVID-19, resulting in death from lung failure [12, 13]. At the same time, scientists and researchers around the globe are working energetically, and data are increasingly generated on the transmission mechanism, the continuum clinical spectrum of disease, new diagnoses, and counteraction remedial systems [14]. In any case, relative deaths from confirmed infection cases were identified for these death rates, and 2 months later, the disease was declared a pandemic by WHO [9, 10]. Until this point, no therapeutics or antibodies are endorsed against any human-contaminating coronavirus [15]. Right now, the best remedial programs and tools for the treatment of COVID-19 are just prevention and forced isolation that helps to reduce the spread of the disease in society [14].
As proven true by the Chinese people in charge, in November 2019, COVID-19 was first transmitted from animal to human working at the open seafood market in Wuhan, and then on 20 January, the disease transmitted from human to human [6, 16]. The virus almost never gains the ability to spread successfully within a new host and a very dreadful sudden onset for the new host infection [17-19]. Coronaviruses come from animals, meaning they are transmitted between humans and animals. Data from a recently published scientific evidence showed that civets transmitted the SARS-CoV virus to humans, and the MERS-CoV virus is transmitted from camels to humans [11, 20]. It has been shown that COVID-19 also crossed animals to infect humans [13]. But the role of bats in virus transmission and the related method of transmission(s) is not yet well understood.
In this brief overview, we summarize basic knowledge of COVID-19, its associated virology, pathophysiology, and histopathology, as well as symptoms, the recommended therapeutic methods, and the suggested vaccines that could provide guidance and future medically useful targets to grasp how COVID-19 co-circulates.
Coronavirus belongs to the Nidoviral Order, Subfamily Orthocoronavirus, Family Oronaviridae, and genus Coronavirus [21]. Coronaviruses are single-strand positive RNA viruses that have a crown-like structure and they replicate in the host cell's cytoplasm [11, 22]. Nidoviral order contains up to four categories of CoVs, namely: Alpha-coronavirus, Beta-coronavirus, Delta coronavirus, and Gamma coronavirus [11]. It has been documented that SARS Cov-2 or COVID-19 is a new member of the genus beta-coronavirus (Figure 1) that is closely connected with the extreme sudden and serious lung-related disease [23].
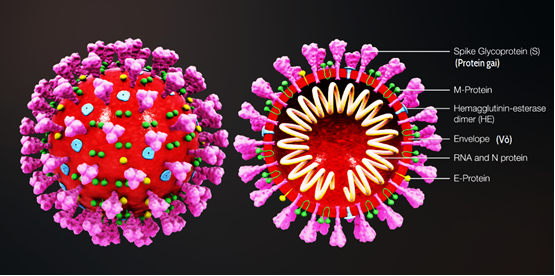
Figure 1: Structure of coronavirus, from https://commons.Wikimedia.org/wiki/file:3D_medical_animation_virus.jpg. Accessed 14 July 2020
SARS-CoV genomic structure is standard coronavirus (Figure 1), with spike (S), replicase (rep), envelope (E), nucleocapsid (N) from the 5P to 3P terminus and membrane (M). Coronavirus envelopes mainly contain three protein types: glycoprotein spike (S), membrane (M and E protein), and non-glycosylated protein envelope (E), but COVID-19 contains one additional protein, i.e., hemagglutinin esterases (HEs). The protein structure in the envelope (Figure 1) plays an important role in the pathogenicity of viruses because it facilitates viral release and assembly [24, 25].
Contrasting other enveloped viruses, CoVs spread and assemble at the endoplasmic reticulum (ER) and Golgi apparatus [26]. Spike protein consists of three components: a large ectodomain, a transmembrane, and a narrow tail, while the ectodomain consists of S1, the amino-terminal receptor binding and S2, the carboxy-terminal membrane fusion (Figure 1). Upon virus entry, S1 binds to a viral attachment receptor on the surface of the host cell, and S2 integrates the host and viral membranes make the virus inside host cells [27, 28]. The E and M are assumed to have a substantial role in viral assembly and the N protein is associated with completing the RNA synthesis [29]. SARS-CoV also encodes some unknown non-structural functional proteins located between M and N; S and E; or below N [23].
The single-strand RNA genome of COVID-19 contains 29891 nucleotides, carrying 9860 amino acid codes [11]. Coronavirus enters the host cells through the transmembrane glycoprotein spike (S) that produces homotrimers on the viral surfaces [28, 30]. S glycoprotein is the primary target of disease-killing antibodies and the subject of a medical diagnosis and immunization program as required for the production of antibodies and the adaptation of host protease that site at the S1-S2 junction [27, 28, 31].
The function of COVID-19 for virulence and pathophysiology is not completely understood, but it is possibly related to the functions of structural and non-structural proteins resulting from genetic mutations [24, 25].
PATHOPHYSIOLOGY
The spike protein binds the host receptors through the angiotensin-converting enzyme2 (ACE2), which can be found across many human organs including the breathing and lung-related system, lymph nodes, gastrointestinal tract, thymus, spleen, bone marrow, liver, brain, and kidney [32, 33]. The most plentiful ACE2 proteins are in type II alveolar cells [34]. The virus then initiates RNA-releasing viral replication in the host cell by developing various virulence factors that will infect more cells and/or inhibit immune response [35]. Additionally, the expression of down-regulating ACE2 leads to local angiotensin II accumulation and activation of the renin-angiotensin-aldosterone system (RAAS), which exacerbates inflammation, disturbs homeostasis, and potentiates tissue damage in the targeted organs [8].
The pathogenic mechanism of pneumonia production appears to be very complicated (Figure 2).
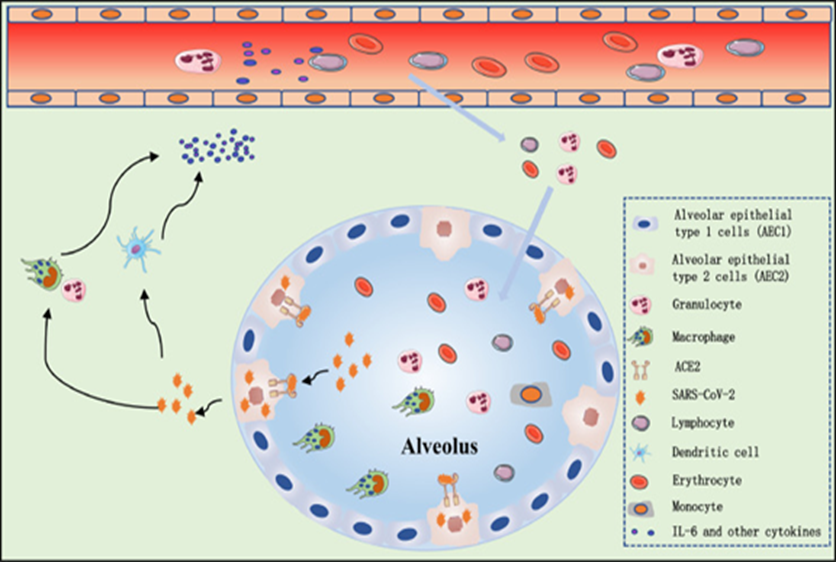
Figure (2): Possible mechanism of cytokines release syndrome in serious COVID-19 patients [8].
The virus can pass through the respiratory tract, and then travel through the lungs and other organs [36]. As ACE2 in bounded to the cell membranes of those organs and not only hydolyses the angiotensin II (a vasconstrictor peptide) into angiotensin 1-7 ( a vasodilator), but also serves as a cell entry point for covid-19 virus [37]. After 7-14 days, the virus starts a second attachment, causing the patient's condition to be irritated Regulation of the immune response is related to the production of adaptive immunity and the severity of diseases [38]. In COVID-19 patients, lymphocytes can slowly decrease as the disease progresses. However, the mechanism of significant lymphocyte reduction is still elusive in patients of the extreme type [39]. However, the inflammatory factors associated with IL-6 diseases were significantly higher, which also led to a worsening of the disease around 2 to 10 days after it began [36].
HISTOPATHOLOGY
The histology of COVID-19 patients’ lung is rare/not enough due to the inaccessible biopsy and autopsy. Histological studies of the lung of the patient who died from SARS-CoV-2 displayed diffuse damage of alveoli and cellular fibromyxoid exudate [32, 33]. The lung, however, displayed a sign of acute respiratory distress syndrome as strong pneumocyte desquamation, the formation of hyaline membrane, and the possibility of pulmonary edema with pulmonary distress syndrome [40]. Enlargement of pneumocytes with large notable nuclei and interstitial inflammatory lymphocyte infiltration with granular amphophilic cytoplasm, and multi-nucleated syncytial cells presented in intra-alveolar on both sides of the lung [41].
Histopathological analysis of the lung biopsy from COVID-19 patients showed widespread alveolar damage, chronic inflammatory infiltrates, pneumocyte hyperplasia in the alveolar lining cells, presence of fibrinous exudates in the intra-alveolar zone, and loose interstitial fibrosis that plugs the intra-alveolar with fibrin in most foci [8].
Post-mortem examination of COVID-19 patients who died from respiratory failure revealed diffuse alveolar damage with severe microthrombi-associated capillary obstruction despite anticoagulation use, in addition to that various changes have been observed in lung and other organs proposing vascular dysfunction [42]. Furthermore, Tian [30] reported that the alterations in the heart and liver and clinical features of COVID-19 patients may be related to the underlying diseases or secondary implication changes.
SYMPTOMS
COVID-19, unlike other coronaviruses, is mainly responsible for the syndrome of respiratory tract infections and its severity can range from mild to fatal due to the onset of pneumonia and serious infection associated with acute respiratory distress syndrome, ARDS [18]. Hence, the clinical symptoms of COVID-19 range from asymptomatic illness to extreme respiratory failure requiring mechanical ventilation and ICU treatment [36].
The most common signs of COVID-19 include dry cough, nausea, and shortness of breath that may be with or without loss of the sense of smell and taste, as well as chills, frequent chill trembling, muscle pain, headache, and sore throat. There is a belief that human corona is related to diseases capable for causing death such as multiple sclerosis, viral hepatitis and infant intestinal disease, but the association between them has not been proven until now [43].
Asymptomatic infections have been documented but their recurrence is elusive and the symptomatic infection tends to be the most serious type of severe pneumonia infection with fever, coughing, and bilateral chest imaging. [36]. As well as that, no particular clinical feature can yet make a reliable distinction between COVID-19 and other viral respiratory infections. Headaches, rhinorrhea, and sore throat include other less common signs. In addition to respiratory symptoms, gastrointestinal symptoms (e.g., diarrhea and nausea) have also been recorded, which may pose a concern in some patients. Respiratory droplet transmission is the main path, and can also be transmitted via personal contacts by asymptomatic carriers [24]
Coronaviruses are a wide group of positive single-strand RNA viruses, which can be isolated from various animal species [44]. It also considers the significant pathogens for the production of episodes of respiratory ailment. For this reason, nucleic acid sequencing testing of respiratory tract samples (rRT-PCR) is required to confirm infection with COVID-19 while the clinical diagnosis is based on signs and symptoms, exposures, and chest imaging [45].
APPLIED THERAPEUTICS
As reported by Lu [46], three general methods are used to identify the possible therapy for human coronavirus, including existing wide-spectrum virus-killing drugs, a compound library containing experimental compounds, and drugs based on the genome and the biophysical understanding for coronaviruses.
Accordingly, the number of antiviral therapies on COVID-19 is being studied, i.e., some investigated agents are either found in observational studies or are anecdotally based on data extrapolated in vitro. The use of these agents is regulated, and COVID-19 is not known for their efficacy. Hence, stressing the efficacy and protection of these agents is necessary [24].
To this end, several randomized trials of various medicines are underway worldwide, as the medical facilities available to investigate new medicinal products that minimize fever, anti-inflammatory or medicinal products used in the past in the treatment of SARS-CoV, MERS-CoV, antimalarial, lupus, rheumatoid arthritis, influenza infection or any other drugs that improve oxygen and allow ventilation in any antiviral drug. Furthermore, a number of antiviral therapies are under review for COVID-19 [24].
Lopinavir/ritonavir
Lopinavir acts as the inhibitor of Human Immunodeficiency Virus (HIV) protease, one of the enzymes that are extremely important to the lifecycle of the virus as well as a cancer-destroying agent for HIV-caused cancers. Although Ritonavir combined with lopinavir through inhibition of cytochrome P45 to increase their plasma half-life P45, it allows a little to no reduction in death among hospitalized COVID-19 patients beyond standard care [47]. Ritonavir/lopinavir does not show any benefit to the primary endpoint beyond regular care, as reported by Stower [48], but it shows benefits to certain secondary endpoints. Potential paths, however, may help confirm or rule out treatment options in patients with serious illness [21].
Remdesivir
Remdesivir is a novel antiviral drug developed for the Ebola virus and Marburg virus infections [49, 50], as it prevents the development of viral infections in human liver cancer [51]. Remdesivir has been reported to inhibit the proliferation of COVID-19 viruses and thus has a clinical potential [19].
Interest in Remdesivir gained traction after its compassionate use helped to treat one of the first patients with critical illness in the United States [19]. Initial results from the comparison of the 5- and 10-day regimen in patients with severe disease suggested no difference in outcomes (clinical recovery, discharge, or death) between the lengths of regimens. However, the conclusion about treatment benefits is limited as there was no control group [52].
Chloroquine and hydrochloroquine
Chloroquine (CQ) and hydrochloroquine (HCQ) are known to be the most active antimalarial drug of the viral disease [53, 54] and have a more or less similar structure and action mechanism [55]. It is also used in treating autoimmune disorders such as lupus and rheumatoid arthritis, HCQ, additionally used in countries where malaria is prevalent. Such medicines are of low cost, fairly effective, and readily available.
Recent research has shown that CQ inhibits in vitro growth of SARS-CoV-2, followed by clinical trials in around 100 patients with SARS-CoV-2 [54, 56]. Because of its ability for tissue penetration including the lung, chloroquine can stop the viral replication within a cell in vitro. Some data showed/told about that HCQ effectively stopped the SARS-Cov-2 entry, transport, and after-entry levels [55].
Human work with HCQ took place in Marseille, France, and found that HCQ alone or in combination with azithromycin was effective in clearing up the nasopharyngeal carriage of viruses within 3 to 6 days [55]. These results indicate that HCQ has a synergistic effect with azithromycin [57]. Nonetheless, several findings and tests did not endorse the use of CQ and HCQ in hospitalized patients reported positive hypoxic pneumonia for COVId-19 [58, 59].
Antibiotic Therapy
The ongoing human trails for COVID-19 is indiscriminate antimicrobial treatment, i.e., combination of antiviral drugs with broad antibiotic range. Therefore, the new NHC guideline suggests INF-α, Lopinavir/ritonavir, and ribavirin [60]. Furthermore, Russell et al. [61] announced that, due to lack of evidence, corticosteroids would not be used in COVID-19 patients..
O2 TherapyThe cure involves only the symptoms, while O2 therapy is the most effective treatment for seriously infected patients [11, 24]. Some counseling focuses on early detection, early isolation, and early diagnosis. Some guidance focuses on early detection, early isolation, and early diagnosis. However, severe and critical cases have been admitted to ICU, and the outpatients for self-isolation and home stay [24, 25]. Furthermore, the WHO advises treating patients with mild signs of sickness and without underlying chronic diseases (such as lung or heart-related disease, kidney-related failure, or immunodeficiency) to be in-home care and in isolation [9]. However, acute and critical cases should be hospitalized and admitted to ICU at the earliest opportunity [29].
VACCINE DEVELOPMENTS
Several candidate vaccines are proposed by an international randomized trial against COVID-19 from private and governmental bodies [9]. Therefore, the removal of COVID-19 is an international priority since without viral spread control the risk of disease would grow with increased mortality every day. Le et al. [62] reported that as of 8 April 2020, the global research and Development technology for COVID-19 included 115 vaccine candidates, 78 of whom were confirmed and 37 were unconfirmed as active trials. Of the 78 confirmed active projects, currently, 73 are in preclinical stages. Recently, the most promising candidates have progressed in clinical research, including Modern's mRNA-1273, CanSino Biologicals' Ad5-nCoV, Inovio's INO-4800 and LV-SMENP-DC, and a pathogen-specific APC from the Shenzhen Geno-immune Medical Center. Several of them, along with many other vaccine manufacturers, have proposed conducting clinical trials in 2020.
CONCLUSION
Our current understanding of COVID-19 disease has put a great deal of pressure on the health and patient care systems. Various methods can be used, depending on the patient's condition and local epidemiology. Demotic treatment is suitable for patients with a symptom. For monitoring patients or suspected patient body temperature, O2 saturation, blood pressure, and breathing signs of sickness for about 14 days. This patient's care will concentrate on avoiding transmission of the virus to others, besides clinical situation observation with hospitalization if feasible. In addition, previous experience in the treatment of COVID-19 by various medicines for Severe Acute Respiratory Syndrome Coronavirus (SARS-Cov), Middle East Respiratory Symptoms (MERS-CoV), Lupus, Anti-Malarial, Influenza Medicine, etc. were used to cure the disease. Nevertheless, the various randomized trials of different drugs underway around the world can be used as a method for tracking the production of CVOID 19 vaccines, and interventions that continue worldwide.
The pharmacodynamics and pharmacokinetic properties and side effects of most medicines exhibiting in vivo and/or in vitro anti-coronavirus properties were not tested in human and animal trials. Most of them are not clinically active because they are associated with immunosuppression or have a value of half of the EC50 anti-coronavirus that is substantially higher than the peak serum concentration (Cmax) that can be obtained at the dose of treatment. Advancing such drugs, however, will cause medicines to turn out to be clinically beneficial alternatives to treatment. Nonetheless, providing authoritative care to patients generally takes quite a long time.
Anyway, many vaccines are proposed by an international (privates and governmental bodies) trial against COVID-19. The elimination of COVID-19 is therefore an international priority, as the risk of disease will increase with increased death every day without viral spread control.
REFERENCES